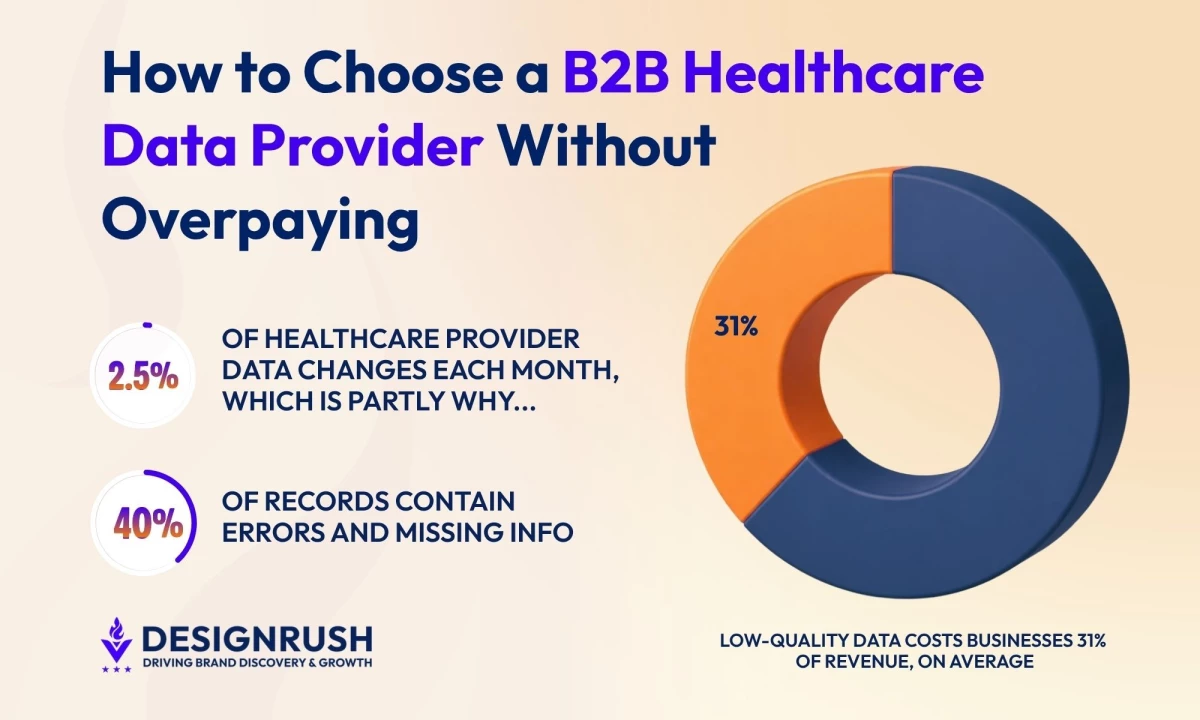
It can feel like B2B healthcare data providers all promise the same thing while hiding wildly different costs and tradeoffs.
To avoid paying for features and platforms that don’t deliver real value, it helps to understand what you really need and how to evaluate your options.
Choosing a B2B Healthcare Data Provider: Key Findings
- Choosing the right B2B healthcare data provider starts with defining your use case and aligning it to the right provider type, rather than comparing tools that solve fundamentally different problems.
- Healthcare data is inherently complex and error-prone (30-40% of healthcare provider records contain inaccurate or missing information) making validation, testing, and fit critical before committing to any vendor.
- The best way to evaluate healthcare data providers is to focus on real outcomes like cost per usable lead and conversion impact.
Understanding Healthcare Data Before You Buy
Healthcare data tends to be fragmented across systems, tightly regulated, and constantly changing. That makes choosing the right provider all about accuracy, relevance, and compliance.
It’s also why healthcare data is more complex (and often more expensive) than standard B2B data. Even basic contact data is harder to verify and keep current due to role changes, multiple affiliations, and compliance constraints.
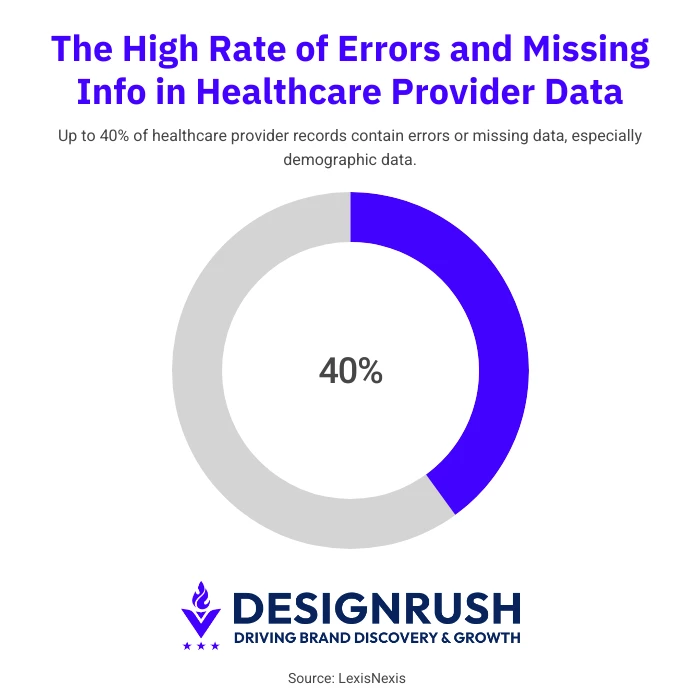
Healthcare provider records (especially demographic data) change continuously, with about 2–2.5% updating each month, according to a report by LexisNexis, alongside frequent shifts in affiliations, status, and sanctions. It follows that 30–40% of healthcare records contain errors or missing data.
On top of that, many providers layer in intent data, but without context, it can add more noise than clarity.
Do You Actually Need External Data?
If you have a well-maintained CRM and clear targeting, internal data may be enough.
There are also free baseline sources, like the NPPES (NPI) registry, which provide foundational healthcare data.
These are useful starting points, but they lack other important administrative contact details outside of registered physicians.
A lack of email addresses, a significant amount of non-practicing (retired) contacts, and inconsistent enrichment attributes mean they are rarely used for revenue-focused use cases on their own.
External data from a B2B Healthcare Data Provider becomes essential when:
- You’re entering new markets or segments
- Your current data is incomplete or outdated
- You need to scale outreach quickly
How to Evaluate B2B Healthcare Data Providers: A Smarter Comparison Framework
Aim to eliminate mismatched vendors early and focus on solutions that actually align with how your team operates.
The most effective way to compare options is to assess B2B Healthcare Data Providers across four core dimensions:
1. Define Your Use Case First
Before looking at B2B Healthcare data providers, get specific about what problem you’re trying to solve. What matters most is how that data will be used in your workflow.
Different use cases require different types of data and levels of precision:
- Lead generation: You need broad coverage and reliable contact data that won’t bounce or go stale quickly
- Enrichment: The focus shifts to match rates and how well external data fills gaps in your CRM
- Sales intelligence: Intent signals, buying triggers, and account-level insights matter more than raw volume
- Analytics: Structured datasets (claims, firmographics, utilization trends) become more important than contacts
Teams lose money by trying to solve all of these with one platform. In reality, most B2B healthcare data providers are optimized for one or two use cases, even if they claim to cover more.
For example:
Platforms like HealthLink Dimensions and MCH Strategic Data are designed for targeted outreach and programmatic activation, using verified provider-level data tied to identifiers like NPIs to reach healthcare professionals across channels
In contrast, companies like IQVIA focus more on large-scale datasets and analytics, often used for market intelligence, clinical insights, or enterprise-level decision-making
Both are “healthcare data providers,” but they solve completely different problems.
2. Match the Right Type of Provider to the Job
Once your use case is clear, the next step is narrowing down what kind of provider you actually need.
Most B2B healthcare data solutions fall into a few distinct categories:
- Data providers / audience data platforms: Companies like HealthLink Dimensions, MCH, or DeepIntent (from programmatic advertising ecosystems) focus on audience targeting and activation, often used by marketing teams.
- Analytics and data infrastructure providers: Companies like Datavant specialize in linking datasets and enabling insights across fragmented systems, rather than providing ready-to-use contact data.
- General B2B data platforms vs healthcare-specific providers: General platforms may offer scale, but healthcare-specific providers tend to deliver better segmentation, compliance handling, and context.
A simple way to think about it:
- If you’re building lists, you’re likely looking at data providers or sales tools
- If you’re improving existing data, enrichment tools are a better fit
3. Decide Your Data Strategy: Build vs Buy vs Hybrid
Not every data problem requires a new vendor. In many cases, the real decision is how much you should rely on external data at all.
There are three practical approaches:
- Build (internal-first): Organizations relying on internal systems (e.g., CRM + first-party data) often focus on maintaining and structuring what they already have, rather than sourcing net-new data. It helps to have strong historical data and defined targeting.
- Buy (external-first): Providers like Komodo Health are usually used when teams need broad market visibility or large-scale datasets, especially for analytics, segmentation, or expansion into new healthcare segments.
- Hybrid (most common): In hybrid setups, providers like MCH Strategic Data are often used to enrich and validate existing CRM data, adding reliable contact details, segmentation, and coverage without requiring a full platform replacement.
A hybrid approach is especially well suited to healthcare since it helps balance coverage (external data) with accuracy and context (internal data).
4. Evaluate Cost Based on Real Outcomes
Pricing in healthcare data gets complicated, and in their confusion, teams often end up overpaying for low-quality data, or data that doesn’t get used.
Common pricing models include:
- Per record or per contact
- Credit-based usage systems
- Per-seat licenses for platform access
- Annual contracts with bundled data and features
Be sure to go beyond the face value of the price offered. Lower cost per record doesn’t mean better value if a large portion of that data is outdated, irrelevant, or unusable.
Failing to prioritize quality and taking the “cheaper option” is one reason low-quality data costs businesses an average of 31% of annual revenue.
A more practical way to assess cost:
- Cost per usable lead: How many contacts actually meet your criteria and are reachable?
- Match rate: How much of the data integrates cleanly with your existing records?
- Downstream impact: Does the data improve conversion rates or just increase volume?
Where teams tend to overpay:
- Buying large datasets when targeting is narrow
- Paying for bundled features (intent, analytics, workflows) that go unused
- Locking into long-term contracts before validating performance
And where higher cost can make sense:
- When accuracy reduces wasted outreach and improves efficiency
- When you need reliable coverage in niche or hard-to-reach healthcare segments
- When compliance and data sourcing standards are essential
Remember, the value of healthcare data isn’t in how much you buy but how effectively it drives pipeline.
As Brian Carter, partner and co-founder of Optymedia, puts it:
“When a company has powerful performance marketing, not just brand marketing, and executives see the value and potential of that, then B2B marketers and salespeople can dramatically boost quality leads and wins.”
5. Understand Compliance, Risk, and Data Usage Boundaries
Healthcare data isn’t just a quality and cost issue, it’s a regulatory one. Choosing the wrong B2B Healthcare Data Provider can expose your organization to legal, financial, and reputational risk.
At a minimum, you need to understand how a provider handles:
- HIPAA and data classification: Not all healthcare data is protected health information (PHI), but if a provider’s data includes or can be linked to PHI, stricter handling requirements apply. You should be clear on whether the data you’re using falls inside or outside HIPAA scope.
- Business Associate Agreements (BAAs): If there’s any chance the data involves PHI, a BAA may be required. If a vendor cannot clearly explain whether a BAA is needed, you’re taking on unnecessary risk.
- Data sourcing and consent: You should understand exactly how the data was collected and whether appropriate consent mechanisms are in place. This is especially important for contact data used in outreach, where regulations like GDPR and CAN-SPAM may apply.
- Usage restrictions: Some datasets are licensed for specific use cases (e.g., analytics vs outreach). Using data outside those terms can create compliance exposure even if the data itself is accurate.
How to Test Healthcare Data Providers Before You Commit
Even if a provider looks like a strong fit on paper, the real test is how their data performs in your workflow. It might be tempting to skip ahead and sign contracts before validating quality, coverage, or usability, but that would be a mistake.
A structured evaluation process helps you avoid long-term commitments based on assumptions.
- The questions you should ask every vendor
- How to run a pilot test (and what metrics to track)
- Vendor evaluation checklist
1. The Questions You Should Ask Every Vendor
Before running any tests, get clarity on how the data is sourced and maintained. Most providers will claim their data is perfectly accurate, but you should pay attention to how they back it up. Vague answers here are usually a red flag.
Focus on these key areas:
Data sourcing and verification
- Where does your data come from?
- How is it collected (self-reported, scraped, aggregated, manually verified)?
- How do you validate accuracy, and how often is the data refreshed?
Coverage specifics
- What does your coverage look like for my target segments (specialties, facility types, geographies)?
- Can you provide examples or sample data for these segments?
- Where is your coverage strongest and where is it limited?
Compliance guarantees
- How do you ensure your data is compliant with healthcare regulations?
- What are the usage restrictions for this data?
- How is consent handled and documented?
2. How to Run a Pilot Test (and What Metrics to Track)
A pilot test is the fastest way to separate strong providers from average ones. The goal isn’t to validate every date point, just to see how the data performs under real conditions.
Start with a small, representative sample and run it through your normal workflow.
View this post on Instagram
2.1 Sample Validation
Manually review a subset (at least 10–20%) of records.
- Are job titles accurate?
- Do contacts align with your ICP?
- Are there obvious gaps or inconsistencies?
If more than 10–15% of records fail basic validation, that’s an early warning sign.
2.2 Bounce Rates (for outbound use cases)
A high email bounce rate is one of the clearest indicators of poor data quality.
- <2% = strong (healthy, high-quality data)
- 2–5% = acceptable but needs monitoring
- >5% = poor data quality and potential deliverability risk
2.3 Match rates (for enrichment use cases)
Measure how much of your existing data the provider can match and enhance. Match rate expectations vary by use case, but in most B2B data workflows:
- >70% is considered strong
- 50–70% is workable
- <50% often limits impact
2.4 Conversion signals
The ultimate test is whether the data drives engagement. Track early indicators like:
- Open rates
- Reply rates
- Meetings booked
3. Vendor Evaluation Checklist
Before committing, you should be able to confidently answer:
- Does this provider perform well for your specific use case, not just in general?
- Is the data accurate and usable, not just large in volume?
- Does coverage align with your target segments and markets?
- Can the data integrate cleanly into your existing workflows and tools?
- Is the pricing justified based on real performance, not just features?
- Is the data sourced, handled, and licensed in a way that meets your compliance requirements?
If any of these are unclear after a pilot, it’s a sign to keep evaluating.
Avoid These Common Mistakes When Choosing a B2B Healthcare Data Provider
Even with a solid evaluation process, it’s easy to make decisions that lead to wasted spend. Most issues come down to misaligned expectations or rushing things.
- Prioritizing database size over relevance: Bigger isn’t better if the data doesn’t match your target. Large datasets often include outdated or irrelevant records, which lowers usability.
- Overvaluing AI and “intent data”: The effectiveness of intent data depends on how well it aligns with your targeting and sales process. Its value depends entirely on how it’s sourced and interpreted.
- Ignoring how healthcare buying actually works: Decision-making in healthcare is rarely tied to a single contact. Roles are distributed across clinical, administrative, and operational stakeholders.
Red Flags That Signal You’re About to Overpay
These are common warning signs that a provider may not be as reliable (or as flexible) as they appear.
- Overpromised accuracy: Claims of near-perfect data quality without a clear explanation of how it’s sourced, verified, or refreshed. If accuracy sounds too good to be true, it usually is.
- Rigid contracts: Long-term commitments with little flexibility on usage, pricing, or scope. This makes it hard to adjust if the data doesn’t perform as expected.
- Lack of transparency: Unclear answers around data sourcing, coverage gaps, or limitations. If a provider avoids specifics, it’s often because the details don’t hold up under scrutiny.
Final Takeaways: How to Choose a B2B Healthcare Data Provider
You’ll need to find the right fit for how your team actually works. The difference in B2B healthcare data providers comes down to clarity around your use case, testing data in real conditions, and evaluating providers based on outcomes, not promises.
By going that route, you'll be far less likely to overpay, and far more likely to end up with data that actually drives results.

Our team ranks agencies worldwide to help you find the right fit. Visit our Agency Directory for the Top Healthcare IT Companies, as well as:
- Top CRM Consultants
- Top Healthcare IT Companies
- Top Marketing Automation Consultants
- Best Cloud Consulting Companies
- Top IT Services Companies In Los Angeles
How to Choose a B2B Healthcare Data Provider: FAQs
1. Is it legal to buy and use healthcare contact data for B2B outreach?
Yes, it is generally legal to use healthcare contact data for B2B outreach, as long as the data is sourced and used in compliance with regulations like HIPAA, GDPR, and applicable marketing laws.
2. What data sources do healthcare data providers actually use to build their databases?
Most providers combine public datasets (like NPPES/NPI), proprietary research, partnerships, web data, and third-party aggregations, often layering verification and enrichment on top.
3. Can you combine multiple lower-cost data tools instead of using one enterprise platform?
Yes, many teams use a combination of specialized tools for sourcing, enrichment, and validation to achieve better flexibility and cost efficiency than a single platform.
4. What internal resources do you need to successfully use a healthcare data provider?
You typically need a well-managed CRM, defined targeting criteria, and some operational capacity to clean, integrate, and act on the data effectively.
5. How long does healthcare B2B data stay accurate before it needs updating?
Healthcare data can degrade quickly (often within months) due to role changes, organizational shifts, and outdated contact details, making regular updates essential.
6. What’s the difference between verified data and enriched data?
Verified data has been checked for accuracy and validity, while enriched data adds additional attributes or context (e.g., missing fields, firmographics, or intent signals).
7. What happens if a healthcare data provider’s data turns out to be inaccurate?
Inaccurate data typically leads to wasted outreach and poor results, and while some providers offer credits or replacements, the real cost is lost time and missed opportunities.